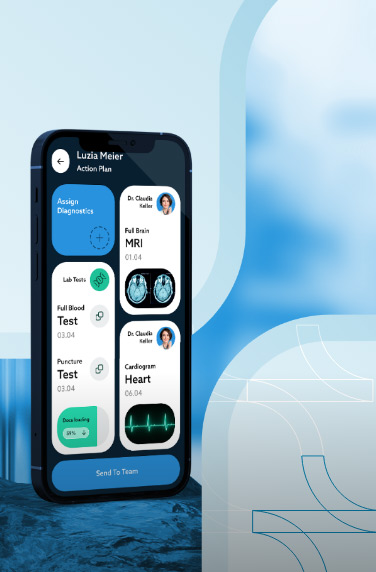
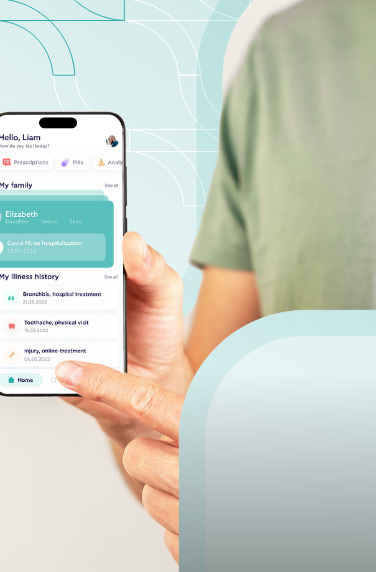
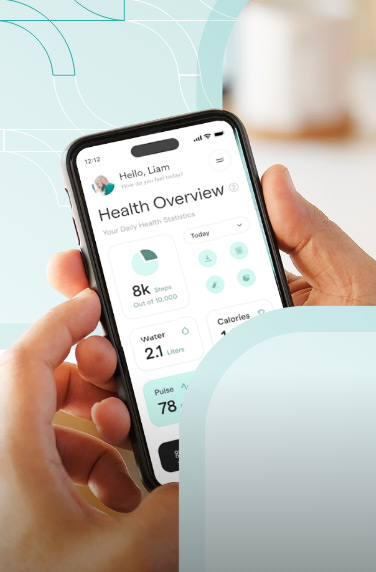
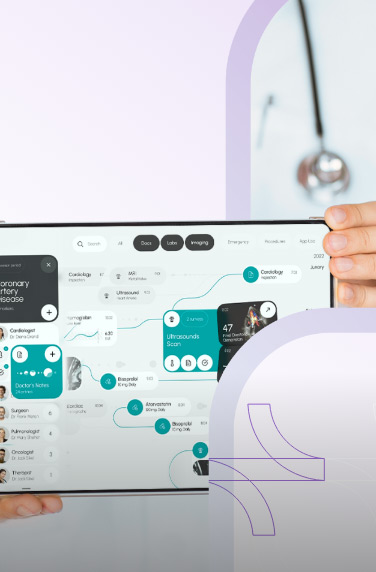
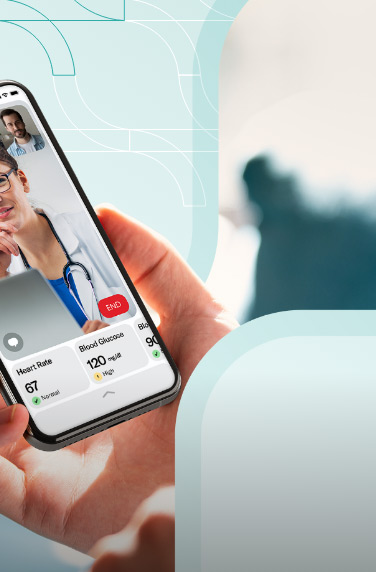
Virtual healthcare, employing technologies like video conferencing, mobile applications, and web-based platforms, provides remote medical care directly to patients.
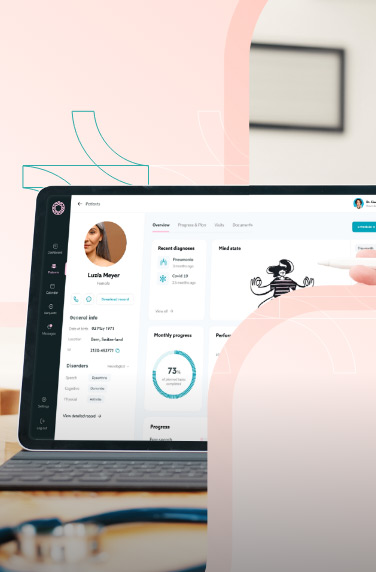
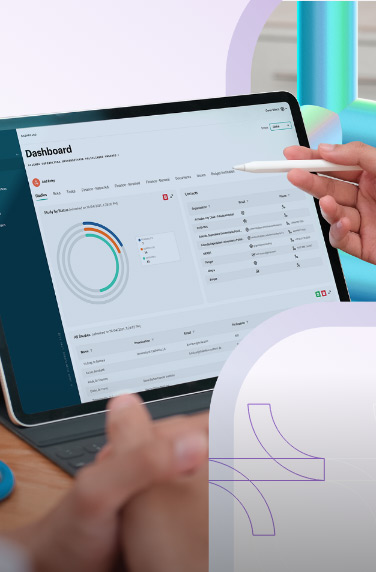
A comprehensive software facilitating video visits enables seamless scheduling of appointments, easy access to medical records, and direct consultations with family medicine doctors or other professionals.
This innovative system transforms the medical industry, offering high-quality care without the necessity of physical hospital or clinic visits.
Telehealth and virtual healthcare both refer to care delivery provided remotely via digital technologies (digital health).
Telehealth is a broader term, encompassing not just clinical services, like video consultations, but also non-clinical services, such as provider training and administrative meetings. It includes a wide array of services like telemedicine, telenursing, and telepsychiatry.
Virtual healthcare, on the other hand, is more specific and focuses on clinical services delivered remotely. It involves real-time interactions between patients and providers, such as virtual consultations, remote monitoring, and digital transmission of medical data.
In summary, while all virtual healthcare is a form of telehealth, not all telehealth is virtual healthcare due to its inclusion of non-clinical services.
Virtual healthcare provides a range of benefits for both patients and providers. One of the significant advantages is convenience. By means of this practice, patients can schedule appointments at their convenience, avoiding the lengthy waiting times often associated with in-person visits.
But did you know that virtual healthcare can also help reduce the spread of infectious diseases? By avoiding crowded waiting rooms and minimizing contact, patients can lower their risk of contracting or spreading illnesses. This fact is highly-relevant during flu season or when dealing with highly contagious diseases like COVID-19.
Furthermore, virtual healthcare enables medical professionals to provide services more efficiently and at a lower cost. Without a physical office or equipment, providers can offer their services at reduced costs, passing on the savings to their patients.
Additionally, virtual practice can help reduce the workload of healthcare professionals, allowing them to focus on providing high-quality care to their patients.
This practice also offers greater accessibility to healthcare services, particularly for individuals living in remote areas or those with mobility issues. For example, sick patients now have access to specialized medical care, such as mental health consultations, without the need to travel long distances.
Last but not least, virtual healthcare has particular significance in chronic condition management. Certain conditions, such as diabetes, heart disease, and cancer, require continuous monitoring, which can be challenging to achieve in traditional settings.
With virtual healthcare, patients can regularly monitor their symptoms and provide remote updates to their physicians. Treating patients with this approach can lead to better management of chronic diseases, thereby improving quality of life.